Colon cancer is increasingly diagnosed in Australians under 50, and symptoms such as rectal bleeding, persistent changes in bowel habits, abdominal pain, unexplained weight loss and fatigue should never be ignored. Early recognition of these colon cancer symptoms under 50 Australia‑wide, especially in people with a family history or lifestyle risk factors, can lead to earlier diagnosis, more effective treatment and better long‑term outcomes. Younger Australians who notice ongoing bowel changes or blood in their stool should speak to their GP promptly and consult reputable resources like Cancer Council and Bowel Cancer Australia for guidance and support.
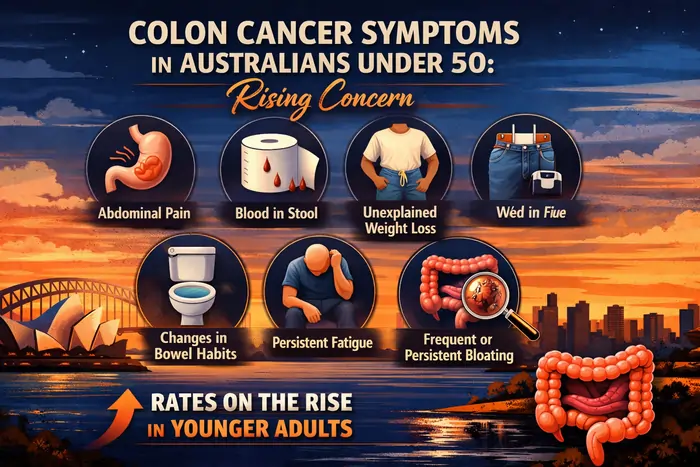
Australia now has some of the highest early‑onset bowel (colon and rectal) cancer rates globally, so recognizing warning signs early and acting on them is critical for people in their 20s, 30s and 40s.
What is colon cancer and why is it rising under 50 in Australia?
Colon cancer (grouped with rectal cancer under “bowel cancer”) begins when the cells lining the colon grow abnormally, forming polyps that can turn into cancer over time. In Australia, overall bowel cancer rates in older people have stabilised or fallen thanks to screening, but cases in adults under 50 have been rising over the last two to three decades.
Researchers believe this increase in early‑onset colorectal cancer is driven by multiple factors: changes in diet, higher rates of overweight and obesity, more sedentary lifestyles, and possible shifts in the gut microbiome and environment. Younger adults are also less likely to undergo routine screening, which means cancers are often diagnosed later, after symptoms have been present for some time.
If you want a deeper breakdown of who is most affected, including age, family history, sex and medical background, the article Who Is Most at Risk of Colon Cancer in Australia? gives a useful Australian‑specific overview.
Why “Color Cancer Symptoms under 50 Australia” is a crucial search
Many Australians under 50 still believe colon cancer is “an older person’s disease” and therefore assume they are too young to worry. This belief is dangerous, because early‑onset cases are increasingly being reported in people in their 20s, 30s and early 40s, including those without a strong family history. When younger people do develop symptoms, they often delay seeking help, or their symptoms are initially attributed to stress, haemorrhoids, irritable bowel syndrome (IBS) or diet.
That’s why searching for colon cancer symptoms under 50 Australia and learning what to watch for is so important. The goal is not to turn every minor symptom into a crisis, but to help you distinguish between short‑lived, harmless issues and persistent red flags that warrant medical review. The Cancer Council’s overview of bowel cancer symptoms is a good companion resource for Australian readers.
Key Color Cancer Symptoms under 50 Australias should never ignore
1. Blood in your stool or rectal bleeding
Blood in the stool is one of the most important warning signs of colon or rectal cancer at any age, including under 50. This may appear as:
- Bright red blood on the toilet paper.
- Blood in the toilet bowl.
- Dark, tarry or maroon‑coloured stools that suggest bleeding higher up in the bowel.
Younger adults often attribute rectal bleeding to haemorrhoids or fissures, especially if they sit for long periods or strain when passing stool. While haemorrhoids are common, any persistent or recurrent rectal bleeding should be assessed by a doctor, particularly when combined with other symptoms like bowel changes or abdominal pain.
You can cross‑check what’s considered a red‑flag symptom in Australia via Cancer Council’s bowel cancer symptoms page and the broader Bowel cancer – Cancer Council Australia resource. For a global medical summary, Mayo Clinic’s page on colon cancer – symptoms and causes also lists rectal bleeding as a key sign.
2. Persistent change in bowel habits
Everyone has occasional bouts of diarrhoea or constipation. Colon cancer is more concerning when the change is new, persistent and unexplained, for example:
- Diarrhoea or constipation lasting for more than a few weeks.
- A noticeable change in how often you go to the toilet.
- Narrow, pencil‑thin or ribbon‑like stools.
- A feeling that your bowels don’t empty fully, even after going.
These changes are especially worrying when they represent a clear departure from your usual pattern, and when there’s no obvious short‑term cause such as a recent infection, travel bug or new medication. Healthdirect provides a plain‑English summary of these bowel changes in its bowel cancer (colon and rectal cancer) information page.
If you notice these colon cancer symptoms under 50 Australia doctors highlight as red flags, it’s worth reading both Healthdirect’s guide and Cancer Council’s bowel cancer symptoms to prepare for a GP visit.
3. Abdominal pain, cramps or bloating
Abdominal discomfort is very common and often benign, but when linked to colon cancer it tends to:
- Persist or recur over weeks to months.
- Be accompanied by changes in bowel habits or bleeding.
- Cause a sense of fullness, cramping or pressure rather than short‑lived “food poisoning” style pain.
Persistent lower abdominal pain, particularly when you can’t link it to a known cause (such as menstrual cycles, IBS, or a clear dietary trigger), deserves attention. Symptom lists on resources like Bowel cancer – Cancer Council Australia and the Mayo Clinic colon cancer page both include abdominal discomfort as a possible sign.
4. Unexplained weight loss and fatigue
Losing weight without trying is another important warning sign, especially when combined with bowel symptoms. Key clues include:
- Weight loss despite your usual eating habits.
- Ongoing fatigue, weakness, or low energy.
- Pale skin, shortness of breath or dizziness, which may reflect anaemia due to chronic internal bleeding.
Younger adults commonly attribute fatigue to work, parenting, study or stress. However, if fatigue is persistent and accompanied by blood in the stool, bowel changes or abdominal pain, you should ask your GP for a thorough check‑up. You can also review broader symptom lists through bowel cancer (colon and rectal cancer) – Healthdirect.
5. Mucus in stool or a feeling of incomplete emptying
Some people with colon or rectal cancer report seeing mucus in their stool, or feeling like they constantly need to have a bowel movement but can’t fully pass anything (tenesmus). While mucus can be part of benign conditions such as IBS or minor infections, persistent mucus or ongoing tenesmus, especially with rectal bleeding, should be discussed with a doctor.
Comparing your own experiences with symptom lists from reputable organisations like Cancer Council’s bowel cancer symptoms can help you decide when it is time to seek care.
6. Anal or rectal discomfort, lumps or pain
Cancers located in the rectum can produce symptoms that overlap with common anal conditions. These may include:
- Pain when passing stool.
- A sense of pressure or a lump in the rectum.
- Persistent anal discomfort or itching that does not resolve.
It’s still important to rule out more serious causes when symptoms linger, recur or are accompanied by other warning signs. Clinicians in Australia often use professional guidance like the RACGP’s colorectal cancer guideline to decide when to refer younger patients for colonoscopy.
Who is most at risk of colon cancer under 50?
Risk is influenced by both factors you can’t change (like genetics) and those you can (like lifestyle). Understanding these helps you know when you may need earlier or closer monitoring.
Non‑modifiable risk factors
You cannot change these, but you should be aware of them:
- Family history: Having a first‑degree relative (parent, sibling or child) with bowel cancer, especially if they were diagnosed under 50.
- Inherited syndromes: Conditions such as Lynch syndrome or familial adenomatous polyposis (FAP) greatly increase lifetime colon cancer risk.
- Personal history: Previous polyps, a past bowel cancer, or inflammatory bowel disease affecting the colon (Crohn’s disease or ulcerative colitis).
- Age and sex: Risk increases with age, but early‑onset cases can affect both men and women; data suggest that a significant proportion of under‑50 cases occur in women.
For an Australian‑focused breakdown of these patterns and how they affect screening decisions, read Who Is Most at Risk of Colon Cancer in Australia?, which explains which groups are considered higher risk locally.
Modifiable lifestyle risk factors
Lifestyle choices play a substantial role in early‑onset colon cancer risk. Some of the most important include:
- Diets high in processed meats and low in fibre.
- High red meat intake, particularly charred or heavily barbecued meat.
- Excess body weight, especially central obesity.
- Lack of regular physical activity.
- Smoking and heavy alcohol consumption.
- Poor sleep patterns and chronic unmanaged stress.
These factors don’t guarantee you will develop colon cancer, but they do shift the odds. The article 12 Lifestyle Choices That Can Increase Colon Cancer Risk walks through everyday habits that significantly influence risk and offers realistic ways to start changing them.
When should Australians under 50 see a doctor?
Because national screening is geared toward people 45 and over, younger adults rely heavily on symptom‑driven detection. You should see a GP as soon as possible if you notice:
- Any rectal bleeding or blood in your stool, especially if it recurs.
- A new, persistent change in bowel habits lasting more than a few weeks.
- Ongoing abdominal pain, cramps or bloating with no clear cause.
- Unexplained weight loss, fatigue or signs of anaemia.
- Persistent mucus in your stool or a constant urge to go (tenesmus).
You should seek urgent or emergency care if you experience:
- Severe abdominal pain and distension.
- Inability to pass gas or stool (possible obstruction).
- Very heavy rectal bleeding, weakness, dizziness or fainting.
Before your appointment, you can prepare by reviewing the symptom lists on Cancer Council’s bowel cancer symptoms page and Healthdirect’s bowel cancer guide, and by noting how long each symptom has been present.
How colon cancer is investigated in younger Australians

When you present to your GP with possible colon cancer symptoms under 50, the usual steps include:
- Detailed history
- Type, duration and pattern of symptoms.
- Family history of bowel cancer, polyps or inherited syndromes.
- Lifestyle factors and other medical conditions.
- Physical examination
- Abdominal exam to check for tenderness or masses.
- Digital rectal examination to detect low rectal tumours or blood.
- Investigations
- Blood tests (including full blood count to check for anaemia).
- Stool tests such as a faecal occult blood test (FOBT) or faecal immunochemical test (FIT).
- Referral for colonoscopy if red flags are present or tests are abnormal.
Colonoscopy remains the gold‑standard test because it allows direct visualisation of the whole colon and rectum and enables polyps or suspicious lesions to be removed or biopsied. Cancer Council’s Bowel cancer – Guide to best cancer care outlines what to expect from investigation through to treatment in Australia.
Screening and early detection in Australia
Australia has a strong, evidence‑based screening program, but it mainly targets older adults. Still, it’s important for younger people to understand how it works:
- The National Bowel Cancer Screening Program sends free at‑home test kits (FIT) to eligible people, currently starting from age 45. You can learn how the kit works and who is eligible via the program’s official pages and this instructional video: How to do the free test – National Bowel Cancer Screening Program.
- Cancer Institute NSW explains how screening invitations are issued and why regular testing matters on its bowel cancer screening page.
- For clinical standards and prevention resources, the Australian Commission on Safety and Quality in Health Care maintains a collection of bowel cancer prevention resources.
If you have a strong family history or other high‑risk features, you may need screening earlier than the general population. This is where understanding your risk via Who Is Most at Risk of Colon Cancer in Australia? is especially helpful.
Reducing your colon cancer risk under 50
Although you can’t modify your genes or family history, you can significantly influence your risk through lifestyle. Some practical steps include:
- Improving your diet: Emphasise vegetables, fruit, whole grains and legumes; reduce processed and ultra‑processed foods.
- Limiting processed and red meat: Especially highly processed products and heavily charred meats.
- Staying active: Aim for regular physical activity most days of the week.
- Maintaining a healthy weight: Even modest weight loss can help if you are overweight.
- Avoiding smoking and moderating alcohol: Both have well‑documented links with bowel and other cancers.
- Managing stress and sleep: Chronic stress and poor sleep can influence hormones and inflammation.
The article 12 Lifestyle Choices That Can Increase Colon Cancer Risk goes into detail on how each of these behaviours affects colon cancer risk and gives practical suggestions for change in an Australian context.
Support and information for Australians under 50
Learning that you might have symptoms of colon cancer or receiving a diagnosis can be overwhelming, especially when you’re under 50 and may have work, children and other responsibilities. There are several reputable support hubs you can turn to:
- Bowel Cancer Australia – central hub for awareness, advocacy, research and patient support: Bowel Cancer Australia.
- Support for you (Bowel Cancer Australia) – tailored help including nurses, dietitians and psychological support for patients and families: Support for you.
- Resource library (Bowel Cancer Australia) – fact sheets, guides and downloadable resources: Resources.
- Cancer Council Australia – comprehensive information on bowel cancer and its symptoms, plus support lines in each state and territory.
- Healthdirect – government‑backed health information on bowel cancer, symptoms and when to seek care.
- Rare Cancers Australia – additional summary and links for people seeking support: Bowel Cancer Australia – Rare Cancers Australia.
After reading about colon cancer symptoms under 50 Australia‑wide, it’s worth bookmarking at least one or two of these sites so you know where to turn if you or someone close to you ever needs more information or support.
FAQs About Colon Cancer Symptoms Under 50 in Australia
Can you get colon cancer in your 20s or 30s in Australia?
Yes. Colon cancer can occur in your 20s and 30s, even without a strong family history. Younger Australians are increasingly being diagnosed, which is why recognising early symptoms is so important.
What are the first signs of colon cancer under 50?
Common early signs include blood in the stool or on toilet paper, a new persistent change in bowel habits, abdominal pain or cramping, unexplained weight loss, and ongoing fatigue. Any combination lasting more than a few weeks should be checked by a GP.
How do colon cancer symptoms under 50 differ from older adults?
The core symptoms are similar, but younger adults are more likely to have symptoms dismissed as IBS, haemorrhoids, or stress. They may also delay care, so cancers are often found at a more advanced stage.
Does blood in the stool always mean colon cancer?
No. Blood in the stool can be caused by haemorrhoids, fissures, or other benign conditions. However, persistent or recurrent bleeding is never “normal” and must be evaluated to rule out serious causes.
How long can you ignore bowel changes before seeing a doctor?
If bowel habit changes last longer than two to four weeks without a clear cause, you should see your GP—especially if accompanied by blood or abdominal pain.
Is colon cancer common in women under 50 in Australia?
Yes. While men have a slightly higher risk overall, many early-onset cases occur in women. Women under 50 should be equally alert to symptoms.
Can IBS or haemorrhoids hide colon cancer symptoms?
They can overlap. IBS causes bowel changes and cramps, while haemorrhoids can cause bleeding. If symptoms change, worsen, or don’t improve, further testing like colonoscopy may be needed.
When should someone under 50 ask for a colonoscopy?
Discuss colonoscopy with your GP if you have persistent red-flag symptoms, a strong family history, or known genetic risk. Your doctor will assess and refer if necessary.
What lifestyle factors increase colon cancer risk in younger Australians?
High intake of processed/red meat, low fibre diet, excess weight, inactivity, smoking, heavy alcohol use, poor sleep, and chronic stress all increase risk.
If my parent had bowel cancer, when should I worry about symptoms?
If a first-degree relative had bowel cancer—especially before age 50—you should monitor symptoms closely and may need earlier screening.
Are colon cancer symptoms always painful?
No. Early-stage colon cancer may cause little to no pain. Subtle signs like mild bleeding or fatigue can appear first.
Can a healthy lifestyle completely prevent colon cancer under 50?
No. A healthy lifestyle lowers risk but doesn’t eliminate it. Genetics and other factors still play a role.
What should I do if I’m embarrassed to talk about bowel symptoms?
Doctors handle these issues every day. You can write symptoms down or start generally—don’t let embarrassment delay care.
Where can younger Australians find reliable information and support?
Trusted resources include Cancer Council Australia, Bowel Cancer Australia, Healthdirect, and state cancer institutes.
What is the prognosis for colon cancer diagnosed early in someone under 50?
When detected early, colon cancer has a high chance of successful treatment and long-term survival. Early action can make a major difference.
